Wellness Tips from Josef Schenker, MD
Welcome to our Wellness Tips blog series, brought to you by Dr. Josef Schenker, the Medical Director at Centers Urgent Care. In this series, Dr. Schenker shares his extensive knowledge and experience in internal medicine and emergency medical services, including folliculitis treatment and prevention, to help you lead a healthier life.
Dr. Schenker will cover a range of crucial health topics, offering expert advice on how to avoid common ailments. With a focus on prevention and practical tips, each blog post is designed to empower you with the information you need to make informed decisions about your health and well-being.
How to Treat Scabies
Scabies affects hundreds of millions of people each year worldwide, with estimates suggesting more than 200 million people have scabies at any given time, and roughly 455 million new cases occur annually. Its treatment focuses on killing the mites with prescription creams or pills, relieving the itch, and stopping the spread to family members or close contacts. In this guide, Dr. Josef Schenker walks through symptoms, timelines, home steps, and when to head in for medical care so you can act early and lower the risk of ongoing skin problems.
Dr. Josef Schenker Explains the Symptoms of Scabies
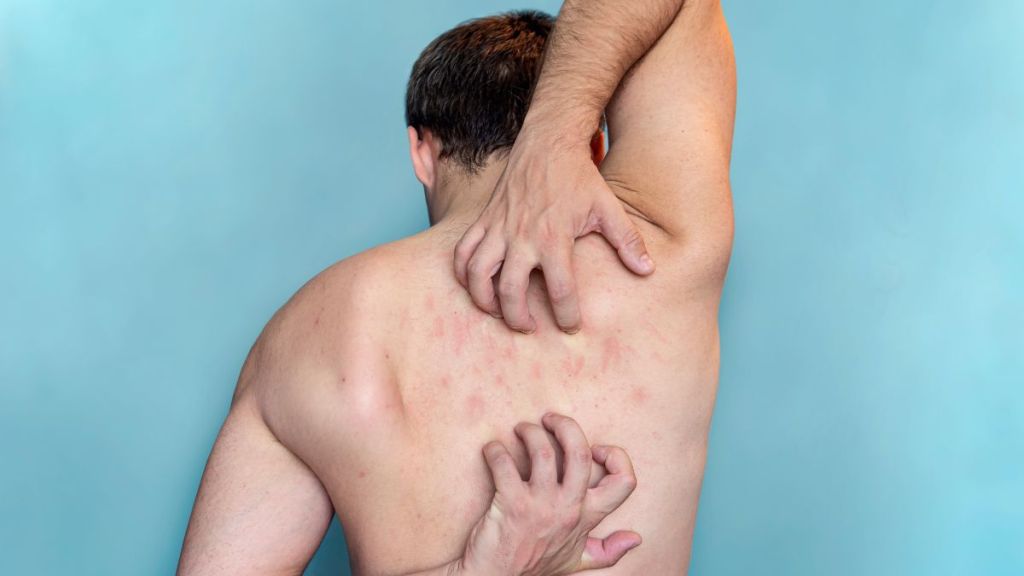
The symptoms of scabies usually show up several weeks after the first mites land on the skin. The immune system needs time to react, so the rash can appear 2 to 6 weeks after exposure, while the person can still pass scabies to others. Its symptoms often look like this:
- Intense itching, especially at night. Many people say the itch feels much worse at night and interrupts sleep. The itching comes from the immune reaction to the mites, their eggs, and their waste, not only from scratching.
- Small red bumps and rash in classic locations. Small, pimple-like bumps or tiny blisters cluster between the fingers, on the inner wrists, elbows, waistline, buttocks, and around the genitals. In infants and young children, the rash can also affect the face, scalp, palms, and soles, so prompt pediatric care is important when a baby or toddler develops a new itchy rash.
- Thin burrow lines on the skin. Fine, wavy, thread-like lines may appear where mites tunnel under the outer layer of skin. These burrows can look gray, skin-colored, or slightly raised and often show up on the sides of the fingers, wrists, or around the navel.
- Crusting or thickened areas in severe cases. Crusted scabies (sometimes called Norwegian scabies) leads to thick, scaly crusts that can hold thousands of mites. This form is more common in people with weak immune systems and needs urgent medical care.
- Scratches, sores, and possible infection. Long-term scratching can break the skin and invite bacteria in, leading to impetigo, folliculitis, and other infections. These sores may ooze, form honey-colored crusts, and increase discomfort.
Josef Schenker, MD, notes that scabies can mimic eczema, contact dermatitis, or simple dry skin, so the combination of night-time itch, typical rash locations, and close-contact spread is a strong signal to get checked.

What Is Scabies?
Scabies is a contagious skin infestation caused by the human itch mite, Sarcoptes scabiei var. hominis. These mites burrow into the outermost layer of skin (stratum corneum) where they lay eggs, triggering a delayed allergic reaction that leads to itching and rash.
Across the world, scabies is recognized as a neglected tropical disease, a major public health concern, and part of the group of common skin infections that spread easily in settings with close, frequent skin contact, such as:
- Households and crowded housing
- Childcare centers and schools
- Nursing homes and long-term care facilities
- Dormitories, prisons, or shelters
Scabies mites cannot fly or jump. They move slowly on skin and pass mainly through prolonged direct contact or, less often, through shared clothing or bedding used shortly before. According to Dr. Josef Schenker, understanding that scabies is an infestation, not just dry skin, helps patients take it seriously and treat both the skin and the environment so the mites do not cycle back.
Can You Stop Scabies From Spreading?
Scabies spread can slow down and stop when both the person with the rash and their close contacts are treated at the same time. Scabies mites usually live on human skin for 1 to 2 months, but survive only about 2–3 days away from the body, which means early treatment and short-term cleaning steps go a long way. These strategies help limit the spread:
- Treat everyone in close contact. Treating all household members, sexual partners, and other close contacts at the same time is essential, even if they do not itch yet. The CDC advises that all close contacts use treatment together to prevent mites from spreading back and forth.
- Limit prolonged skin-to-skin contact until treatment is complete. This is especially important in homes, dorms, and care facilities.
- Handle clothing and bedding correctly. Wash clothing, bedding, and towels used during the three days before treatment in hot water at or above 50°C (122°F) for at least 10 minutes, then dry on a hot cycle or dry-clean them. Items that cannot be washed can be placed in sealed plastic bags for several days to a week.
- Plan for group settings. In schools, nursing homes, or similar settings, coordinated treatment and environmental cleaning greatly reduce outbreaks. Some large outbreaks use oral ivermectin under medical supervision for many residents at once.
- Remember that hygiene alone is not enough. Regular bathing does not remove mites once they are under the skin. Real control comes from prescription scabies treatment plus careful handling of clothes and bedding during the first days of care.
How Long Does Scabies Last?
The duration of the condition depends on when treatment starts, the type of scabies present, and whether reinfestation occurs. Josef Schenker, MD, points out that the mites can be killed quickly with correct treatment, but the itch can linger even after the mites are gone. Here is a simple guide to typical timelines:
- Untreated classic scabies. Classic scabies will continue indefinitely without treatment, as mites keep laying eggs and new mites hatch.
- After proper scabies treatment. Medicines that kill mites (scabicides) usually clear the mites within a day of treatment.
- Itch after treatment. Itching and rash often last 2 to 4 weeks after successful treatment because the skin continues to react to dead mites and their waste.
- Crusted or severe scabies. Crusted scabies may require multiple treatments over several weeks with both oral and topical medicines and close follow-up, especially in people with weak immune systems.
If new burrows or fresh itchy bumps appear after 2 to 4 weeks, or if more family members start to itch again, a doctor should reassess for reinfestation or another skin condition.
Josef Schenker, MD, Explains How to Treat Scabies
Scabies treatment aims to kill mites, calm the skin, and prevent spread to others. As Josef Schenker explains, both the prescription medicine and its use are important. Common treatment steps include:
- Use prescription scabicides as directed. First-line treatment for most people is permethrin 5% cream applied from the neck down and left on for 8–14 hours before washing off.
- Consider oral ivermectin in certain cases. Oral ivermectin can be used for crusted scabies, large outbreaks, or when topical treatment fails. Typical regimens use at least two doses, spaced 7–14 days apart, under medical supervision.
- Apply cream to all required areas. Cream usually needs to cover the entire body from the neck down, including between fingers and toes, under nails, under breasts, around the genitals, and between buttocks.
- Relieve itching and skin irritation. Oral antihistamines, mild topical steroids, and soothing moisturizers can ease itching while the skin settles.
- Treat secondary infections if present. If there are open sores or signs of bacterial infection, doctors may add antibiotics or special creams to help the skin heal and lower the risk of deeper infection.
No over-the-counter product in the United States is currently approved to treat scabies on its own, so treatment should always involve a healthcare professional who can choose the right medicine and give clear instructions.
How to Avoid Getting Scabies
Scabies prevention focuses on limiting close contact with active cases and acting quickly if someone in the household develops a new rash or hives. Hygiene is useful but does not replace treatment. These habits help reduce the chance of getting scabies:
- Be cautious with prolonged skin contact. Long, close skin contact, such as sleeping in the same bed or sexual contact with someone who has scabies, greatly raises the chance of getting mites.
- Respond early in group settings. Schools, dorms, long-term care facilities, and shelters should act promptly upon suspicion of scabies.
- Watch for outbreaks in high-risk communities. Scabies is more common in crowded living conditions and in communities with limited access to water or health services. Awareness of this helps families and staff act quickly when a new itch or rash appears.
- Treat everyone at once when a case is confirmed. When a doctor confirms scabies, treating everyone in the same household at the same time is among the strongest preventive measures to prevent new cases and reinfestation.

What to Do if Someone Has Scabies
Scabies in a family member or roommate calls for organized but simple steps. The goal is to treat the skin, clean the environment for a short period, and protect others from catching the mites. Josef Schenker reminds patients that quick action lowers stress and shortens the period of itching. Here are practical steps to take right away:
- Call a healthcare provider for diagnosis and treatment. A doctor or other qualified provider can usually diagnose scabies by examining the rash and may confirm it with a skin scraping or other lab work if needed. They will prescribe the right scabies treatment cream or pill and explain how to use it.
- Follow the application instructions carefully. Apply the prescribed cream to all required areas of the body and leave it on for the recommended time before washing it off. Repeat the treatment if told to do so, often about a week later.
- Discourage scratching and watch for infection. Keep nails trimmed, consider using cotton gloves at night for children, and use provider-recommended anti-itch medicines. New sores that look yellow, swollen, or painful should be checked for possible bacterial infection.
Most people can return to work, school, or childcare 24 hours after starting treatment, once the first application of medicine is complete and clean clothes are worn. You can visit an urgent care clinic whenever the rash is severe, crusted, spreading quickly, or causing sleep loss; if there are signs of infection; or if someone in the home has a weak immune system.
Centers Urgent Care can evaluate a suspicious rash, confirm if it is scabies or another condition, prescribe scabies treatment medicines, and guide your family on cleaning steps and follow-up so everyone recovers sooner.
Josef Schenker, MD, Answers Frequently Asked Questions
Can scabies go away on its own without treatment?
No, scabies does not usually go away on its own. Mites continue to live and reproduce in the skin without treatment. Prescription creams or pills are needed to fully eliminate the infestation and prevent it from spreading.
How should I clean my home and clothes after scabies treatment?
After scabies treatment, wash all clothing, bedding, and towels used in the past three days in hot water (at least 50°C/122°F) and dry on high heat. Seal unwashable items in plastic bags for several days, and vacuum carpets and furniture to remove any remaining mites.
Can I get scabies from my dog or cat?
in humans, but cannot survive or reproduce on human skin. Pets with mange need veterinary care, and humans with lasting symptoms should consult a doctor.
What happens if scabies is left untreated?
If left untreated, scabies causes persistent itching, skin damage from scratching, and the risk of bacterial infections like impetigo. In high-burden areas, repeated infections may lead to complications such as kidney disease or rheumatic heart disease. Prompt treatment prevents these outcomes and stops the spread.
When should I go to urgent care for scabies?
You should go to urgent care for scabies if you have intense night itching with a new rash, can’t access your regular doctor, or need a diagnosis. Seek prompt care for crusted scabies, spreading sores, fever, or if you’re immunocompromised or caring for high-risk individuals.

Focus on Early Care: Protect Your Household from Scabies
Scabies treatment works best when the rash is recognized early, everyone in close contact is treated together, and the home environment is cleaned for a short window. In this article, you learned how scabies starts, how long it can last, and what practical steps make treatment more effective and prevent new cases.
You can visit our urgent care facility in New York for a same-day exam if you suspect scabies or another itchy rash. Centers Urgent Care offers convenient access to evaluation, diagnosis, and scabies treatment options that fit your situation. Under the leadership of Dr. Josef Schenker, our team helps patients understand their treatment, protect family members, and lower the risk of repeat infestations.
We operate multiple locations across NYC to make walk-in care easier when an itch and rash get in the way of daily life. Locate a Centers Urgent Care near you.

About Josef Schenker, MD:
Dr. Josef Schenker, a board-certified expert in internal medicine and emergency medical services, brings extensive experience and compassion to his role as Medical Director and Partner at Centers Urgent Care. With leadership in SeniorCare Emergency Medical Services and as an Attending Physician at New York-Presbyterian Brooklyn Methodist Hospital, Dr. Schenker oversees critical care and treatment protocols across varied medical needs. His dedication extends to chairing NYC REMAC, ensuring adherence to state standards in emergency medical procedures. At Centers Urgent Care, Dr. Schenker's expertise ensures prompt, high-quality emergency care for patients of all ages, supported by state-of-the-art facilities including a dedicated pediatric suite.