Wellness Tips from Josef Schenker, MD
Welcome to our Wellness Tips blog series, brought to you by Dr. Josef Schenker, the Medical Director at Centers Urgent Care. In this series, Dr. Schenker shares his extensive knowledge and experience in internal medicine and emergency medical services, including hand-foot-and-mouth disease treatment and management, to help you lead a healthier life.
Dr. Schenker will cover a range of crucial health topics, offering expert advice on how to avoid common ailments. With a focus on prevention and practical tips, each blog post is designed to empower you with the information you need to make informed decisions about your health and well-being.
Hand-Foot-and-Mouth Disease Treatment and Management at Home
Hand-foot-and-mouth disease (HFMD) can derail a week of school, work, and sleep with fever, painful mouth sores, and a fast-spreading rash. Most people recover in 7–10 days. Spread moves quickly in childcare and classrooms. For scale, the Centers for Disease Control and Prevention (CDC) estimates 10–15 million non-polio enterovirus infections in the U.S. each year; and HFMD is one subset of those infections. HFMD is most common in children under 5 and tends to rise in summer and early fall.
To give context, recent U.S. reports show the spread without one national count each year. Fairfax County, VA had six outbreaks in 2025, West Virginia saw clusters in schools and daycares, and the U.S. Virgin Islands reported 189 cases. Up ahead, Dr. Josef Schenker will give more insights and set the plan for care and recovery.
Dr. Josef Schenker Explains the Symptoms of Hand-Foot-and-Mouth Disease
This disease follows a simple arc. Early cold-like signs show up first, then mouth sores, then a rash. According to Dr. Josef Schenker, watching the order helps you respond early and prevent dehydration at home. Here’s a look at its symptoms:
- Fever. This often arrives first, about 3 to 5 days after exposure. It can be low to moderate and may last a couple of days. Track temperature against pediatric vital signs.
- Sore throat and flu-like feelings. Aside from making swallowing uncomfortable, children may seem worn out and want to rest more.
- Mouth sores (ulcers). These are small red spots in the mouth and can turn painful. Sores tend to appear on the tongue, gums, and inner cheeks.
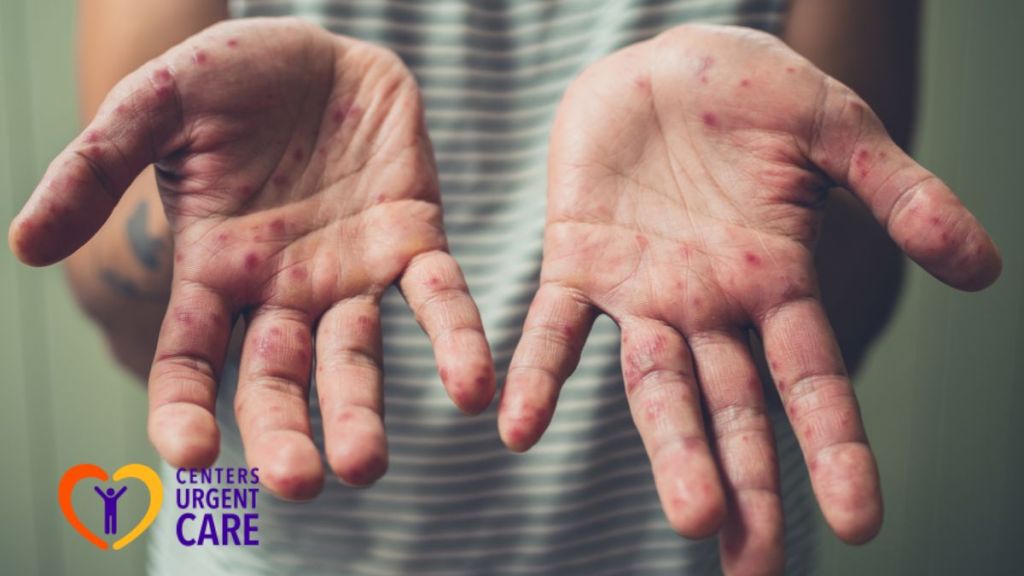
- Skin rash on hands and feet. A rash appears on the palms and soles and can also show on the buttocks, legs, and arms. Spots are flat or slightly raised, and some become small blisters.
- Painful swallowing and drooling. Young children may drool more because swallowing hurts. They often prefer cold fluids and avoid acidic foods.
- Decreased appetite and drinking less. Kids may eat and drink less in the first days of illness.
- Irritability and sleep disruption. Discomfort from fever, sores, and rash can make infants and toddlers fussy. Naps may be shorter, and nights can be restless.
- Signs of dehydration. Watch for dry mouth, fewer tears, and fewer wet diapers or trips to the bathroom. Dark urine or no urine for 6 to 8 hours needs prompt attention.
- Nail changes weeks later (uncommon). A small number of children shed fingernails or toenails a few weeks after HFMD. Nails grow back on their own. Reports describe this as rare and usually harmless.
Not every child shows every sign. Some children have a mild rash and a few mouth sores, while others have more obvious symptoms. Adults can get HFMD too, though the illness is often milder.

What Is Hand-Foot-and-Mouth Disease?
Hand-foot-and-mouth disease is a viral illness that causes fever, mouth sores, and a rash on the hands and feet. It spreads easily in close contact settings. As Dr. Josef Schenker explains, the illness is uncomfortable but usually mild and short. Most people recover at home.
HFMD comes from several enteroviruses. Coxsackievirus A16 is the typical cause in the United States. Coxsackievirus A6 can also cause HFMD and may bring more intense symptoms. Enterovirus A71 appears less often in the U.S. but has been linked to neurologic complications in some outbreaks abroad.
Transmission happens through day-to-day contact. The viruses spread via respiratory droplets, saliva and nasal fluids, fluid from blisters, stool, and contaminated surfaces.
A quick note: HFMD is not the same as the livestock illness foot-and-mouth disease (FMD). Different viruses cause them, and FMD is an animal disease that does not pose a routine human health threat.
Can You Stop Hand-Foot-and-Mouth Disease Once It Starts?
You can’t stop HFMD after symptoms begin. There is no specific antiviral medication that clears the infection. Care centers on comfort and watchful home care until the illness runs its course.
There is also no U.S.-licensed vaccine for the viruses that cause HFMD. Research vaccines exist elsewhere, but none are available in the United States today. That is why prevention relies on hygiene and smart isolation practices.
The practical goal in this phase is simple. Keep the child comfortable and avoid choices that worsen symptoms. Supportive care is the standard approach endorsed by leading pediatric and primary care groups.
How Long Does Hand-Foot-and-Mouth Disease Last?
This disease is short. Most people recover in 7–10 days, with no special medicines needed. Symptoms peak early, then ease on their own. As Josef Schenker, MD explains, knowing the typical timeline helps you plan care at home and set school or work expectations.
- Typical course by symptom. Fever comes first and improves within 2–3 days. Painful mouth sores and throat pain follow and usually settle by about a week. The hand-and-foot rash can linger a bit longer but clears within the 7–10 day window for most patients.
- Contagious window. People are most contagious during the first week. Virus can still shed for days to weeks after symptoms fade, especially in stool.
- Return to school or child care. Children may attend when they have no fever, feel well enough to participate, and are not drooling uncontrollably from mouth sores. Local health rules may vary during outbreaks.
If symptoms persist beyond the usual window or hydration is hard to maintain, a quick in-person check helps. At Centers Urgent Care, we offer same-day walk-ins. You can visit us for an exam, a hydration assessment, and a practical return-to-school note if needed.

Josef Schenker, MD, Explains Hand-Foot-and-Mouth Disease Treatment and Management
This is a supportive disease, meaning the aim is to keep kids comfortable while the illness runs its course. Josef Schenker, MD highlights three goals for home care: relieve pain, protect hydration, and keep skin comfortable. Here are the core treatment steps for HFMD:
- Pain and fever medicines. Use acetaminophen or ibuprofen based on age and weight to ease fever and soreness. Follow dosing instructions on the label or from your clinician. Do not give aspirin to children because of the risk of Reye syndrome.
- Hydration strategy. Offer frequent small sips to avoid dehydration when the mouth is sore. Oral rehydration solutions are useful during illness; they replace fluids and salts lost when kids drink less.
- Mouth care and food choices. Cool liquids and soft foods go down easier when ulcers hurt. Avoid hot, spicy, salty, or acidic items that sting open sores and slow intake. Brushing with gentle toothpaste that does not irritate the mouth may also help.
- Skip numbing gels and sprays. Avoid benzocaine-containing gels in infants and young children, and steer clear of viscous lidocaine for oral pain. The FDA warns these products can be harmful and offer limited benefit for mouth pain. Focus on systemic pain relief and cool fluids instead.
- Skin and blister care. Keep the skin clean with gentle soap and water. Do not pop blisters. Intact skin lowers infection risk, and blisters usually heal on their own. If a blister breaks, wash the area and cover it with a clean bandage.
- What medicines won’t help. Antibiotics do not treat HFMD because viruses cause it. There is no specific antiviral medicine for routine cases, so treatment focuses on comfort. Most people improve without prescription drugs.
Not every child needs every step. Some kids only need fever control and quiet time, while others need more help with drinking and mouth pain.
How to Avoid Hand-Foot-and-Mouth Disease
Prevention starts with daily habits. Small changes at the sink and on shared surfaces cut spread in homes and classrooms. As Josef Schenker notes, focus on clean hands, clean surfaces, and no sharing of items that touch the mouth. Here are practical steps that work:
- Wash hands with soap and water. Handwashing for 20 seconds after diaper changes, bathroom trips, and before eating lowers risk in close-contact settings. Regular handwashing can reduce respiratory illnesses by around 21% and diarrhea by up to 30%, which helps during HFMD season.
- Disinfect high-touch surfaces and toys the right way. Use an EPA-registered disinfectant or a properly diluted bleach solution, and follow the label exactly. For best results against enteroviruses, choose products with claims against nonenveloped viruses (for example, norovirus or poliovirus).
- Don’t share cups, utensils, or personal items, and avoid face-touching. Viruses that cause HFMD spread through saliva and nasal fluids and enter through the eyes, nose, and mouth. Sharing cups, utensils, towels, or toothbrushes gives germs an easy route. Teaching kids to keep hands away from their face adds another simple barrier.
- Practice cough and sneeze etiquette, then wash up. Covering coughs and sneezes with a tissue or elbow reduces droplets on shared surfaces. Used tissues go straight into the trash, followed by handwashing.
- Use strict diapering and bathroom hygiene. Caregivers should wash hands after every diaper change and help children do the same after bathroom use. Diapering areas, potty chairs, toilets, and sinks need cleaning and disinfection on a set schedule and whenever soiled.
- Plan a classroom routine for mouthed toys and shared gear. Mouthed toys should be removed, cleaned, and disinfected before reuse. High-touch items such as doorknobs, light switches, and tablet screens need daily attention.
Quick tip for staff meetings: Posting a “Wash for 20 seconds” card at sinks and a short checklist near the cleaning supplies keeps everyone aligned on the basics.

What to Do if Someone Has Hand-Foot-and-Mouth Disease
When HFMD shows up at home, keep the plan simple. Focus on comfort, fluids, and limiting spread. Here are the action steps to follow:
- Check hydration first. Mouth pain cuts drinking, so watch urine output and energy. Offer frequent small sips and use oral rehydration drinks if intake dips. Seek care if drinking stays poor or dehydration signs appear.
- Use short home isolation and plan a return. Keeping kids home while a fever is present or drooling from mouth sores is hard to control. Return when there is no fever, they can take part in class, and drooling is under control.
- Simplify comfort care. Offer cool liquids and soft foods that are easy to swallow. Skip acidic or spicy choices that sting.
- Clean what hands touch most. Have everyone wash hands often, especially after diaper changes and before eating. Wipe high-touch items and toys; clean first, then disinfect as the label directs.
- Know the “see a clinician now” cues. Call or visit if fever lasts more than 3 days, symptoms are severe, your child is very young, or symptoms do not improve by 10 days. Seek medical attention sooner if you notice signs of dehydration, such as not urinating for 8 hours or having a very dry mouth.
- If you head to urgent care, bring basics. Pack a list of medicines and allergies, plus the timing of last fluids and fever doses. A clear list speeds safe care and reduces mix-ups.
Josef Schenker, MD, Answers Frequently Asked Questions:
HFMD is contagious for about 7 days during the first week of illness. The virus persists in stool for up to 4 weeks, in throat secretions for 3 weeks, and in blisters until healed. Transmission can occur even after recovery, so strict hygiene helps prevent spread.
Avoid acidic foods like citrus, soda, and tomato, spicy or salty items, rough crunchy textures, and hot drinks with HFMD because they worsen mouth sores. Choose soft, cool foods such as yogurt, applesauce, smoothies, and mashed potatoes, while emphasizing fluids to ease swallowing and prevent dehydration.
Yes, you can bathe a child with hand, foot, and mouth disease. Lukewarm baths with mild soap keep skin clean and reduce infection risk. Avoid scrubbing or popping blisters, pat skin dry, and launder towels after each use. Normal bathing does not spread HFMD, but strict hand hygiene remains essential.
A child with HFMD should stay home until the fever resolves and the child feels well enough to participate, with drooling from mouth sores under control. Blisters do not need to heal before return. Some schools may require exclusion during outbreaks, so check local policy while maintaining strict hygiene.
Ice cream is good for HFMD because cold, soft foods soothe mouth pain and make swallowing easier. Choose ice cream, sherbet, or ice pops, but avoid citrus or acidic flavors that sting. If dairy worsens diarrhea, use non-dairy cold options. Hydration with chilled fluids remains the main priority.
Yes, you can go to urgent care for HFMD if a child cannot drink well, shows dehydration, has a fever for over 3 days, is very uncomfortable, or has symptoms that last beyond 10 days. Infants under 6 months and immunocompromised children should be seen promptly. Most cases improve at home with fluids and pain relief.
Trusted Care for Hand-Foot-and-Mouth Disease
Hand-foot-and-mouth disease often runs its course in about a week, but symptoms like painful mouth sores, fever, and rashes can make recovery difficult, especially for young children. With careful home management and the right medical guidance, most families can keep children comfortable and prevent complications.
At our urgent care facility in New York, patients receive timely evaluations and treatment plans tailored to their needs. The experienced team at Centers Urgent Care focuses on comfort, hydration, and supportive care so families can manage symptoms effectively and return to normal routines.
Led by Dr. Josef Schenker, our providers are committed to giving each patient reliable care and practical solutions when illness disrupts daily life. Locate a Centers Urgent Care near you and get trusted care today.

About Josef Schenker, MD:
Dr. Josef Schenker, a board-certified expert in internal medicine and emergency medical services, brings extensive experience and compassion to his role as Medical Director and Partner at Centers Urgent Care. With leadership in SeniorCare Emergency Medical Services and as an Attending Physician at New York-Presbyterian Brooklyn Methodist Hospital, Dr. Schenker oversees critical care and treatment protocols across varied medical needs. His dedication extends to chairing NYC REMAC, ensuring adherence to state standards in emergency medical procedures. At Centers Urgent Care, Dr. Schenker's expertise ensures prompt, high-quality emergency care for patients of all ages, supported by state-of-the-art facilities including a dedicated pediatric suite.

