Wellness Tips from Josef Schenker, MD
Welcome to our Wellness Tips blog series! With decades of experience in both emergency and internal medicine, Dr. Josef Schenker is here to simplify the path to better health. At Centers Urgent Care, we believe wellness should feel achievable and not overwhelming, so this series focuses on practical advice that’s easy to follow and impactful. Whether you’re dealing with a specific health concern or simply looking for ways to enhance your daily routine, these tips are crafted with your well-being in mind.
Managing Tendonitis
Tendonitis is a common condition, especially for those who engage in repetitive motions or overuse specific parts of their bodies. Whether you’re an athlete, an office worker, or someone who performs manual labor, tendonitis can sneak up on you, making everyday tasks painful and challenging.
In this article, Dr. Josef Schenker will break down the details of tendonitis, from its causes to treatment options, and offer expert advice on how to manage and prevent this condition.
Dr. Josef Schenker Explains What is Tendonitis
Tendonitis occurs when a tendon, the thick cord that attaches muscle to bone, becomes inflamed or irritated. Tendons play an essential role in movement, but they can become strained or overused, leading to this painful condition. Tendonitis can affect any tendon in the body, but it most often strikes the shoulders, elbows, wrists, knees, and heels. Those who are most at risk include athletes, older adults, and people whose jobs require repetitive motions.
Josef Schenker, MD stresses that it’s important to recognize the signs early and take steps to treat them before it worsens. Luckily, tendonitis is typically treatable with proper care and rest, and most people recover fully with time and the right interventions.
Types of Tendonitis
There are several types of tendonitis, each affecting different areas of the body. Here are some of the most common types:
- Rotator cuff tendonitis (shoulder): This type of tendonitis affects the tendons in the shoulder, usually from repetitive overhead movements or lifting. Athletes, such as swimmers and baseball players, often suffer from this.
- Tennis elbow (lateral epicondylitis): Commonly seen in tennis players and individuals who perform repetitive wrist and arm motions, tennis elbow affects the tendons on the outside of the elbow, causing pain and weakness.
- Golfer’s elbow (medial epicondylitis): Similar to tennis elbow, golfer’s elbow affects the tendons on the inside of the elbow. This condition results from repetitive gripping or bending of the wrist.
- Achilles tendonitis (heel): The Achilles tendon connects the calf muscles to the heel bone. Achilles tendonitis is common among runners (affecting 30% of all runners) and those who increase their physical activity suddenly.
- Patellar tendonitis (jumper’s knee): This type affects the tendons around the kneecap and is common in basketball players (12%), volleyball players (14%), or anyone engaging in repetitive jumping activities.
- De Quervain’s tendonitis (thumb): This type occurs in the tendons on the thumb side of the wrist, causing pain when gripping or twisting.
Causes of Tendonitis
Tendonitis often results from repetitive motion or overuse, but other factors can contribute to the condition as well. Here are the most common causes:
- Repetitive activities: Engaging in the same motion repeatedly, such as typing, painting, or sports activities, can put a strain on tendons, leading to inflammation.
- A sudden increase in physical activity: A rapid increase in exercise intensity, such as jumping into a new workout routine without proper conditioning, can overstress tendons.
- Age-related wear and tear: Tendons lose elasticity with age, making them more prone to injury and inflammation, especially in older adults.
- Improper technique or equipment: Using incorrect form while exercising or poorly fitting sports equipment can put additional strain on tendons, leading to tendonitis.
- Injury or trauma: A sudden impact or twist can damage tendons, leading to inflammation and pain.
- Underlying conditions: Conditions like rheumatoid arthritis or diabetes can make tendons more susceptible to injury or inflammation.
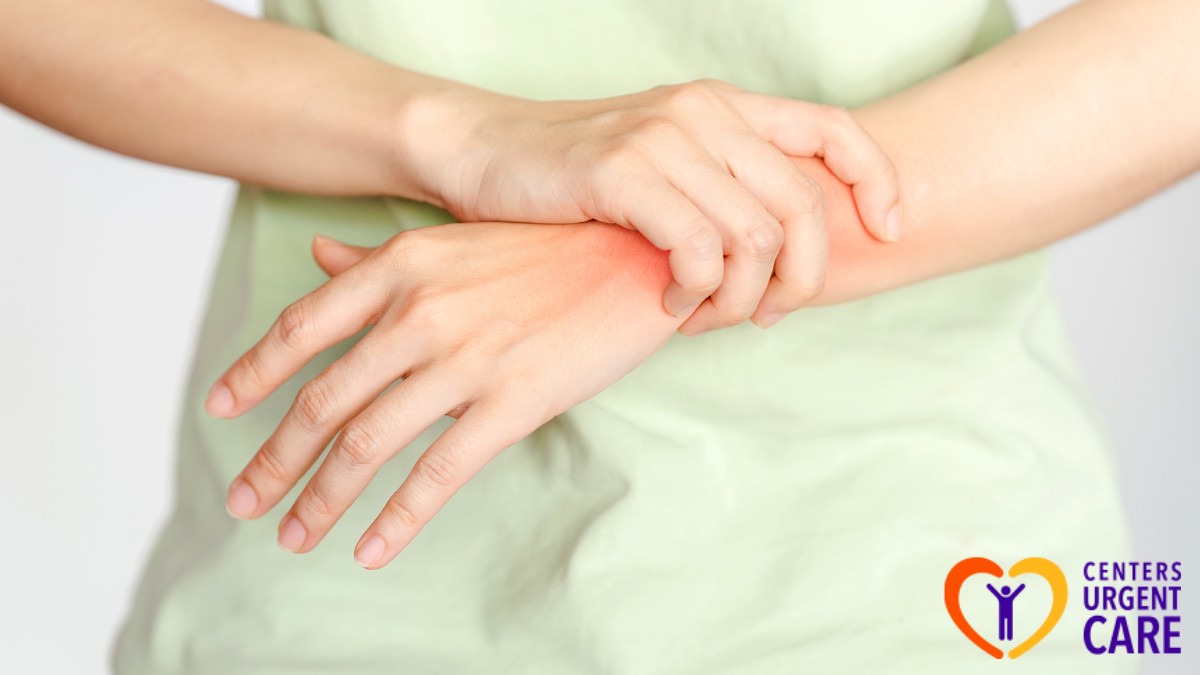
Symptoms of Tendonitis
Tendonitis symptoms vary depending on which part of the body is affected, but they typically involve discomfort around joints and muscles. Here’s what to look for:
- Pain at the site of the tendon: Pain is the most common symptom and can range from a dull ache to sharp pain, especially when moving the affected joint.
- Tenderness and swelling: The area around the tendon may become swollen and sensitive to touch.
- Stiffness: Tendonitis can cause stiffness, especially after periods of inactivity, making it hard to move the affected joint.
- Loss of strength: Tendonitis often leads to weakness in the affected area, making tasks that require strength, like lifting or gripping, more difficult.
- Limited range of motion: As the tendon becomes inflamed, you might find it harder to move the joint through its full range of motion without discomfort.
These symptoms typically affect areas such as the shoulders, elbows, wrists, knees, and heels. If you notice any of these signs, especially after repetitive motion or overuse, it’s important to take action early to prevent the worsening of the condition.
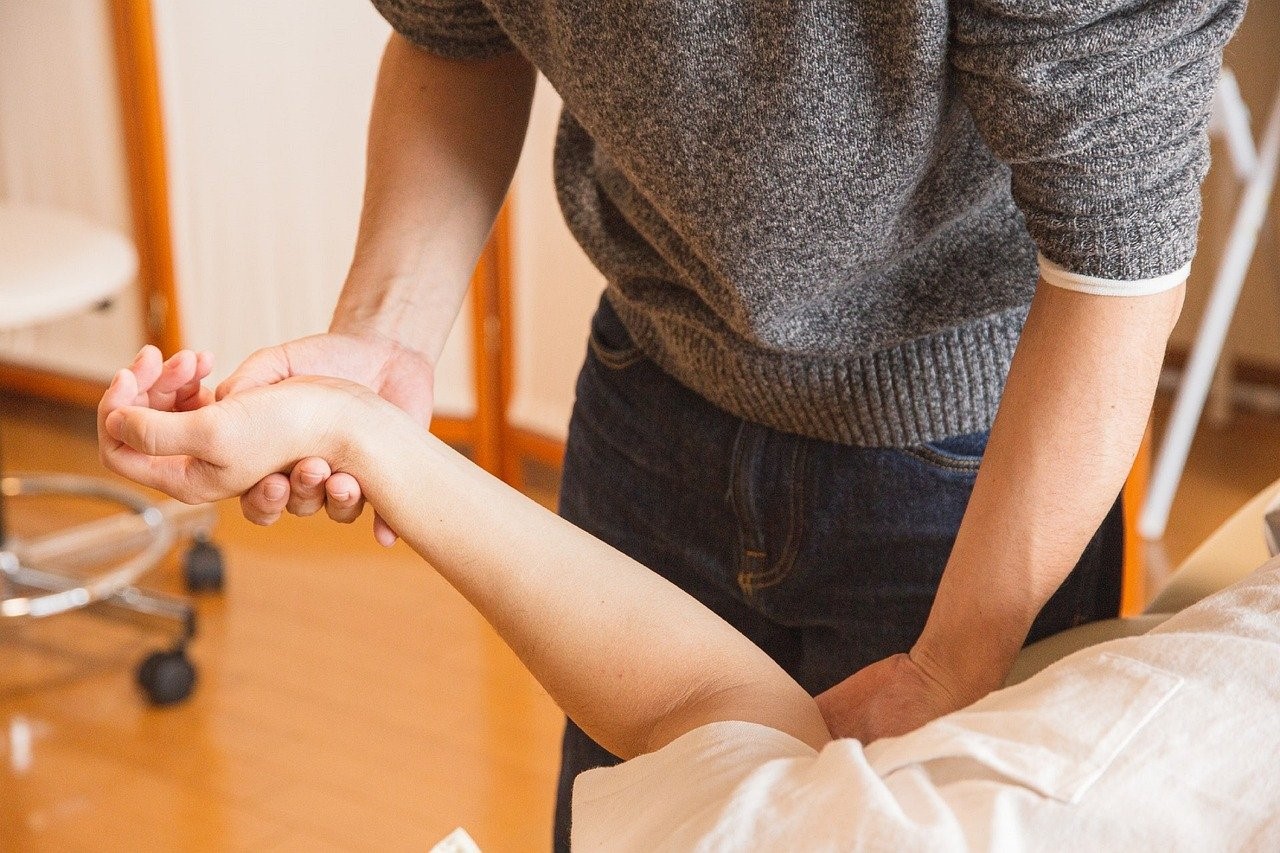
Josef Schenker, MD, Explains the Proper Management and Treatment of Tendonitis
Managing tendonitis requires a combination of rest, proper care, and sometimes medical treatment. The goal is to reduce inflammation, alleviate pain, and allow the tendon to heal without further damage. Here are the most common treatment approaches for tendonitis:
- Rest: The first and most important step is to rest the affected tendon. Avoid activities that exacerbate the pain to give the tendon time to recover.
- Ice therapy: Applying ice to the affected area can reduce inflammation and numb the pain. Use ice packs for 15–20 minutes, several times a day.
- Compression: Wrapping the affected area with an elastic bandage can help control swelling and stabilize the tendon.
- Elevation: Keeping the affected limb elevated, especially after injury or flare-up, can reduce swelling and pain.
- Medications: Over-the-counter pain relievers such as ibuprofen or naproxen can help reduce pain and inflammation. In more severe cases, a doctor may prescribe stronger anti-inflammatory medications or corticosteroid injections.
- Physical therapy: A physical therapist can guide you through exercises that strengthen the muscles around the tendon and improve flexibility, helping to prevent future flare-ups.
- Splinting or bracing: For certain types of tendonitis, such as tennis elbow or De Quervain’s tendonitis, wearing a brace or splint can help support the tendon and reduce strain.
- Surgery: Surgery is rarely needed for tendonitis, but in severe cases where other treatments don’t work, a surgeon may need to remove damaged tissue or repair the tendon.
Recovery can take several weeks or even months, depending on the severity of the condition. According to Josef Schenker, the key is to be patient and consistent with treatment.
How to Prevent Tendonitis?
While tendonitis can’t always be avoided, there are several steps you can take to reduce your risk and protect your tendons. Prevention is particularly important if you’ve had tendonitis before or engage in activities that put you at higher risk.
- Warm up before physical activity: Warming up properly helps prepare your tendons and muscles for activity, reducing the risk of injury.
- Use proper technique: Whether you’re exercising or performing daily tasks, using the correct form and technique can help avoid overstraining tendons.
- Strengthen supporting muscles: Strengthening the muscles around the tendons can reduce stress on the tendons themselves, lowering your risk of inflammation.
- Take breaks from repetitive activities: If your job or hobby involves repetitive motions, make sure to take regular breaks to give your tendons a chance to rest.
- Stretch regularly: Regular stretching helps improve flexibility and reduces the risk of tendonitis, especially in areas prone to tightness, like the shoulders and calves.
- Maintain good posture: Poor posture can put unnecessary stress on your tendons, particularly in your neck, shoulders, and back.
- Gradually increase activity levels: Avoid sudden increases in exercise intensity, and give your tendons time to adapt by gradually increasing the demands you place on them.

Josef Schenker, MD, Answers Frequently Asked Questions:
What is the difference between tendonitis and arthritis?
Tendonitis is the inflammation of a tendon, often caused by repetitive use, resulting in pain and limited movement. Arthritis, on the other hand, involves inflammation of the joints, leading to pain, stiffness, and swelling, affecting overall joint function and mobility.
How long does tendonitis heal?
Tendonitis typically takes a few weeks to several months to heal, depending on the severity and location of the condition. Adhering to rest, ice, compression, and elevation (RICE) protocols, along with physical therapy, can significantly aid in recovery time.
Is heat or ice better for tendonitis?
Ice is generally better for tendonitis, especially in the acute phase, as it helps reduce inflammation and numb pain. Heat can be beneficial for chronic tendonitis to relax and loosen tissues, but it’s essential to apply it at the right time.
When to seek medical advice for tendonitis?
Seek medical advice for tendonitis if pain persists despite home treatment, worsens over time, or interferes with daily activities. Additionally, consult a healthcare professional if you notice swelling, redness, or a fever, as these may indicate a more serious condition.

Overcome Tendonitis Pain
Tendonitis doesn’t have to limit your daily activities. By recognizing the signs early, taking preventive measures, and following the right treatment plan, you can manage tendonitis effectively and get back to the activities you enjoy.
If you’re struggling with tendon pain, don’t wait—reach out to any of the Centers Urgent Care facilities across New York. Our competent team of medical professionals led by Dr. Josef Schenker can provide the diagnosis and treatment you need for a speedy recovery. With the right care, you can overcome tendonitis and protect your tendons for the long run!

About Josef Schenker, MD:
Dr. Josef Schenker, a board-certified expert in internal medicine and emergency medical services, brings extensive experience and compassion to his role as Medical Director and Partner at Centers Urgent Care. With leadership in SeniorCare Emergency Medical Services and as an Attending Physician at New York-Presbyterian Brooklyn Methodist Hospital, Dr. Schenker oversees critical care and treatment protocols across varied medical needs. His dedication extends to chairing NYC REMAC, ensuring adherence to state standards in emergency medical procedures. At Centers Urgent Care, Dr. Schenker's expertise ensures prompt, high-quality emergency care for patients of all ages, supported by state-of-the-art facilities including a dedicated pediatric suite.

MY HERPES STORY AND HOW I WAS CURED
For years, I struggled with the emotional and physical burden of the herpes virus, believing I would have to live with it forever. I tried countless treatments, medications, and therapies, but nothing seemed to bring lasting relief. It felt like a battle with no end in sight until I discovered a natural remedy that changed everything (herbs). Skeptical at first, I decided to give it a try, and to my surprise, I started noticing improvements in my overall well-being within two days of taking the medication. With consistency as prescribed by the herbal doctor, I felt healthier, more energized, and free from the symptoms that had once controlled my life. After completing the treatment, (14days) I visited my doctor for confirmation, and I was overjoyed with the results. I tested negative. I was cured from my HSV1&2
This experience has given me back my confidence, peace of mind, and a renewed sense of hope. If you or someone you know is struggling with herpes or other health concerns like HPV, endometriosis, ovarian cysts, PCOS, or hepatitis, know that there are alternative options available and you will be cured. For those seeking a natural approach to wellness, I encourage you to explore this path with an open mind. You never know how life-changing it might be. Just if you want to reach out, you can contact:
Email: dr.awaseherbalhome@gmail.com
WhatsApp: +2349074997110